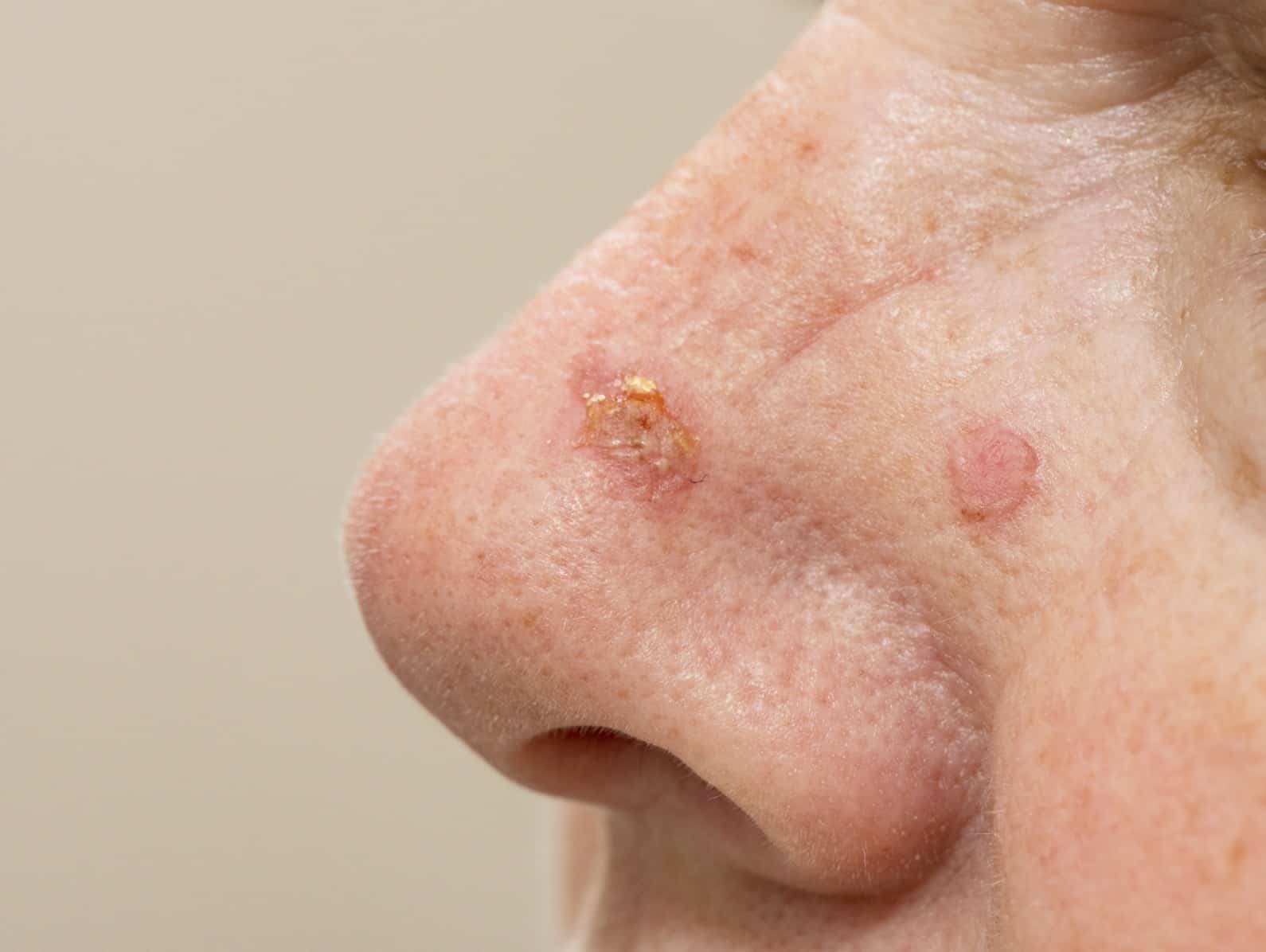
Solar (actinic) keratosis
Solar keratoses are premalignant lesions (the epidermal basal cell layer is dysplastic) that
indicate chronic sun damage and are a marker of the risk of developing skin cancer.
About 20% regress spontaneously. Progression of single lesions to SCC is uncommon
(<1/1000 per annum). Areas of coalescing solar keratoses on sun-damaged skin, i.e.
‘actinic field change’, have a higher risk of progression to SCC, particularly in the
context of immunosuppression.
What should I look for?
• Asymptomatic or slightly itchy, brownish red, discrete scaly/keratotic patches on sun-
exposed skin: bald scalp, face, helix of the ear, dorsum of the hands, and forearms.
• Some may be raised and warty: hypertrophic solar keratosis.
• Pain, induration, inflammation, or ulceration (suggests progression to SCC). Signs of
chronic sun damage, including skin tumours: BCC, SCC, malignant melanoma.
What should I do?
• Advise patients to monitor their skin for development of skin cancers and to protect
their skin from the sun.
• Treatment, e.g. cryosurgery, is only required if keratoses are troublesome. Topical
treatments are effective for confluent areas of field change, e.g. topical diclofenac,
fluorouracil, imiquimod, ingenol mebutate, or photodynamic therapy.
Bowen disease (SCC in situ)
Characterized by full-thickness epidermal dysplasia. Peak incidence in seventh decade.
Only about 3–5% of plaques progress to SCC—but the risk of metastasis from SCC is
increased. Aetiologies: chronic sun exposure (including sunbeds), radiation, oncogenic
HPV (HPV-16 associated with anogenital, palmoplantar, and periungual SCC in situ),
immunosuppression, and arsenic (lesions in sun-protected areas). Plaques are
asymptomatic and enlarge slowly over years. Often misdiagnosed as ‘discoid eczema’ or
‘ringworm’ but fails to respond to treatment for these conditions.
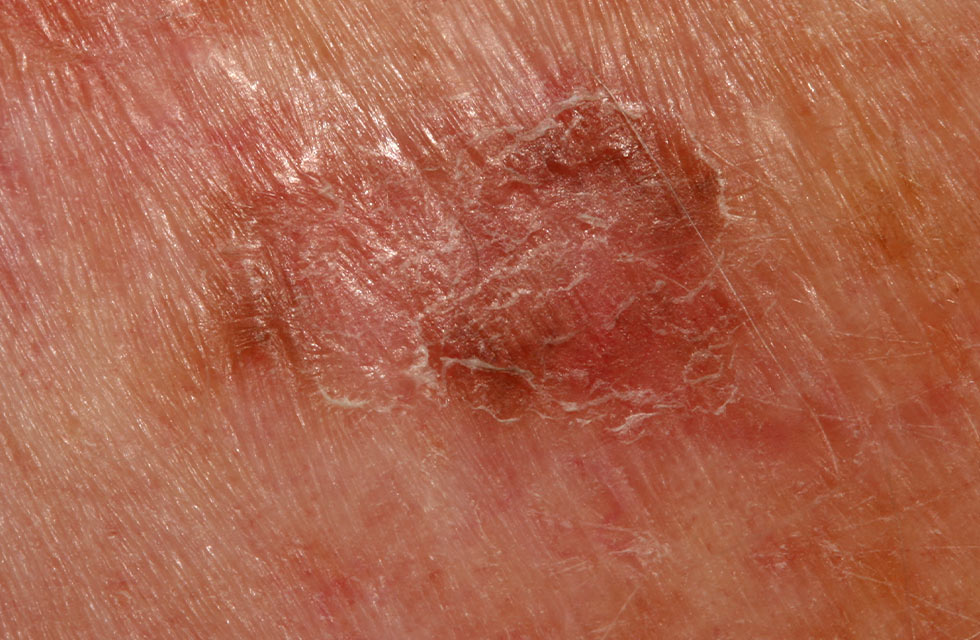
What should I look for?
• A well-defined erythematous scaly or warty plaque.
• A flat edge: stretch the skin gently, and inspect the edge closely. A raised thready
border suggests a superficial BCC, rather than Bowen disease.
• Dermoscopy shows glomerular vessels (focal nests of tortuous vessels resembling
vessels in the renal glomerulus) with scaling.
• Nodularity or ulceration: this may indicate progression to SCC.
What should I do?
• Take a skin scrape to exclude a fungal infection, if indicated.
• Take a skin biopsy to confirm the diagnosis.
Treatment options include surgical removal (shave excision), topical fluorouracil, topical
imiquimod, or photodynamic therapy. Patients should protect their skin from the sun