
1. WHAT IS A ‘VASCULAR BIRTHMARK?’
Many babies have what are called ‘birthmarks’ when they’re born. In some cases they may appear within the first few weeks of life. They can be brown, tan, blue, pink, or red. More than 10 in 100 babies have vascular birthmarks.
These are made up of blood vessels bunched together in the skin. They can be flat or raised, pink, red or bluish discolorations.
2. WHAT CAUSES BIRTHMARKS?
Why do vascular birthmarks occur? The exact causes are unknown. Most vascular birthmarks are not inherited, nor are they caused by anything that happens to the mother during pregnancy.
3. WHAT ARE THE DIFFERENT TYPES OF VASCULAR BIRTHMARKS?
There are different kinds of vascular birthmarks. Sometimes, the birthmark must be watched for several weeks or months before the specific type can be identified. The most common types of vascular birthmarks are macular stains, hemangiomas, and port wine stains. There are also many rare types of vascular birthmarks.
Macular Stains
-
Your physician will call faint, mild red marks macular stains. They are the most common type of vascular birthmarks. They are also called ‘angel’s kisses,’ when they are located on the forehead or eyelids. When they’re found on the back of the neck, they’re called ‘stork bites.’ They may also occur on the tip of the nose, upper lip or any other body location. They are pink and flat. Angel’s kisses almost always go away by age two, but stork bites usually last into adulthood. These birthmarks are harmless and require no treatment.
Hemangiomas
-
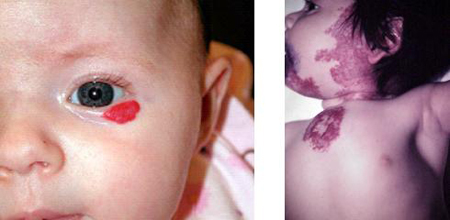
The term ‘hemangioma’ is used to describe many different kinds of blood vessel growths. Most dermatologists prefer to use hemangioma to refer to a common type of vascular birthmark. These marks do not usually appear immediately after birth, but become visible within the first few weeks of life.
-
Hemangiomas are usually divided into two types: strawberry hemangiomas and cavernous hemangiomas.
-
A strawberry hemangioma is slightly raised, and bright red because the abnormal blood vessels are very close to the surface of the skin.
-
Cavernous hemangiomas have a blue color because the abnormal vessels are deeper under the skin. Hemangiomas are more common in females and in premature babies. They can be anywhere on the face or body.
-
Usually, a child will have only one hemangioma, but sometimes there will be two or three. In rare cases, an infant may have many, or even some internally. Unlike other vascular birthmarks, hemangiomas can grow very rapidly. Growth generally begins during the first six weeks of life and continues for about one year. Most never get bigger than two or three inches in diameter, but some may be larger. After the first year, most hemangiomas will stop growing. They then begin to turn white and slowly shrink. Half of all hemangiomas are flat by age five; nine out of ten are flat by age nine. Many will completely go away, but often, a faint mark is left. It’s impossible to know how big any hemangioma will grow, or if it will completely disappear.
-
Complications of Hemangiomas
-
Occasionally, a hemangioma that’s growing or shrinking rapidly can form an open sore or ulcer. These sores can be painful, and can become infected. It’s very important to see your dermatologist and keep this sore clean and covered with antibiotic ointment and/or a dressing.
-
A hemangioma located over the female genitals or rectum, or near an eye, the nose or mouth, can cause special problems. These hemangiomas should be watched closely by your dermatologist who will decide if further treatment is necessary.
-
Parents are often concerned that a hemangioma will bleed. These birthmarks do look as if they could bleed easily. However, this usually isn’t a problem. Bleeding usually occurs only after injury. If the hemangioma starts to bleed, it should be treated like any other injury–clean the area with soap and water or hydrogen peroxide and apply a gauze bandage. Apply firm, but not tight, pressure on the area for five to ten minutes. If the bleeding has not stopped, call your doctor.
-
A hemangioma will rarely grow suddenly over one or two days. If this occurs, it’s important to call your dermatologist. Also, if a bruise begins to develop, your dermatologist should be notified.
-
Treatment of Hemangiomas
-
It’s very important that a baby with a vascular birthmark be examined by a dermatologist as early as possible, so that a correct diagnosis can be made and the need for treatment discussed.
-
It’s not always easy for parents to watch a hemangioma grow, or wait for it to disappear, without doing anything. However, most hemangiomas do not require treatment. They eventually shrink by themselves, leaving very few signs.
-
There are several different types of treatments for hemangiomas that need care. No treatment is absolutely safe and effective. The potential benefits must be weighed against the possible risks.
-
The most widely used treatment for rapidly growing hemangiomas is corticosteroid medication. This is either injected or given by mouth. Long-term or repeated treatment may be necessary. Some of the risks of therapy include poor growth, elevated blood sugar and blood pressure, cataracts and an increased chance of infection.
-
Lasers Fraxel Laser can be used to both prevent growth of hemangiomas and remove hemangiomas. Hemangiomas with sores that will not heal can also be treated with lasers. New lasers are being developed and studied by dermatologists to treat this condition.
Port-Wine Stains
-
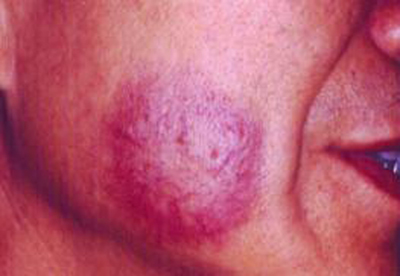
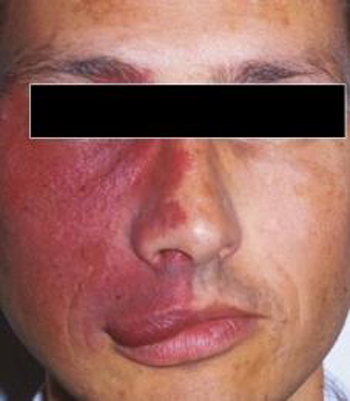
The port-wine stain is another type of vascular birthmark that occurs in 3 in 1,000 infants. It is sometimes called a nevus flammeus, or capillary hemangioma, but it should not be confused with a hemangioma.
-
Port-wine stains appear at birth. They are flat, pink, red or purplish discolorations, found most often on the face, neck, arms or legs. They can be any size. Unlike hemangiomas, port-wine stains grow only as the child grows. Over time, port-wine stains may become thick and develop small bumps or ridges. Port-wine stains do not go away by themselves. They last a lifetime.
-
Port-wine stains, especially those on the face, can have emotional, social, and economic complications. Port-wine stains on the forehead, eyelids or both sides of the face, can be associated with glaucoma is increased pressure within the eye that, left untreated, can cause blindness. These complications occur in less than one-fourth of those with port-wine stains of the forehead and eyelids. All infants with a port-wine stain in those areas should have a thorough eye and brain examination.
-
Occasionally, there may be very gradual enlargement of tissues surrounding a port-wine stain. All children with large port-wine stains involving an arm or leg should be followed for any growth problems.
-
With time, port-wine stains can develop small blood vessel growths, called pyogenic granulomas. These can bleed easily, and should be removed.
-
Treatment of Port-Wine Stains
-
The use of cover-up makeup has been a common treatment for port-wine stains. Your doctor can provide you with more information about products that are made to cover up birthmarks
-
Various methods have been tried in the past to remove port-wine stains, but none have worked well. New types of lasers have shown the best results with the least amount of risk and side effects. Laser treatment Fraxel Laser of port-wine stains is FDA-approved, and available at many centers around the country. For best results, treatment should begin as early as possible, even in infancy. Laser surgery is performed on an outpatient basis. Several treatments are usually required, given at two month intervals. Younger patients often require fewer treatments than adults. In about one-fourth of the patients, lasers can totally clear up the port-wine stain. Seventy percent will look much better. For reasons that are not understood, a small number of patients will not respond well to laser therapy.
-
There are several risks of laser therapy. An increase or decrease in skin color can occur, leaving patchy tanning or whitening of the skin. In most cases this is not permanent. Swelling, crusting or minor bleeding can occur. This is unusual and can be treated easily. Permanent scarring has happened, but is extremely rare. Laser therapy is uncomfortable, but not extremely painful. Anesthesia is not required for most adults. However, anesthesia is often important for toddlers and young children. If putting the child to sleep is required, there are some risks and higher costs.
-
Most vascular birthmarks disappear without treatment or can be treated effectively. Through research, dermatologists are learning more about the causes and treatments of all types of vascular birthmarks.