Pathogenesis is poorly understood. Malassezia furfur (pityrosporum ovale), a lipophilic
yeast that is a skin commensal is found in large numbers in involved skin. Reaction to the
yeasts may play some part in the pathogen- esis. Adult seborrhoeic dermatitis is chronic
and recurrent. Parkinson disease and epilepsy predispose to seborrhoeic dermatitis.
Patients with hIV/AIDS may have very severe disease. Although seborrhoeic dermatitis
is not particularly itchy, it is disfiguring. Infantile seborrhoeic dermatitis is unrelated to
the disease in adults.
What should I look for?
One or more sites may be affected:
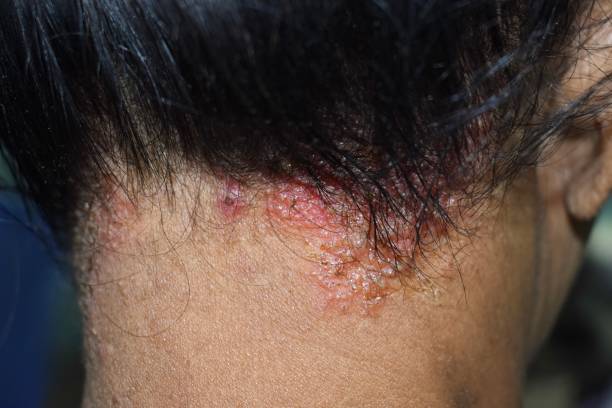
• Poorly defined scalp erythema and fine white scale (dandruff). Hair is retained.
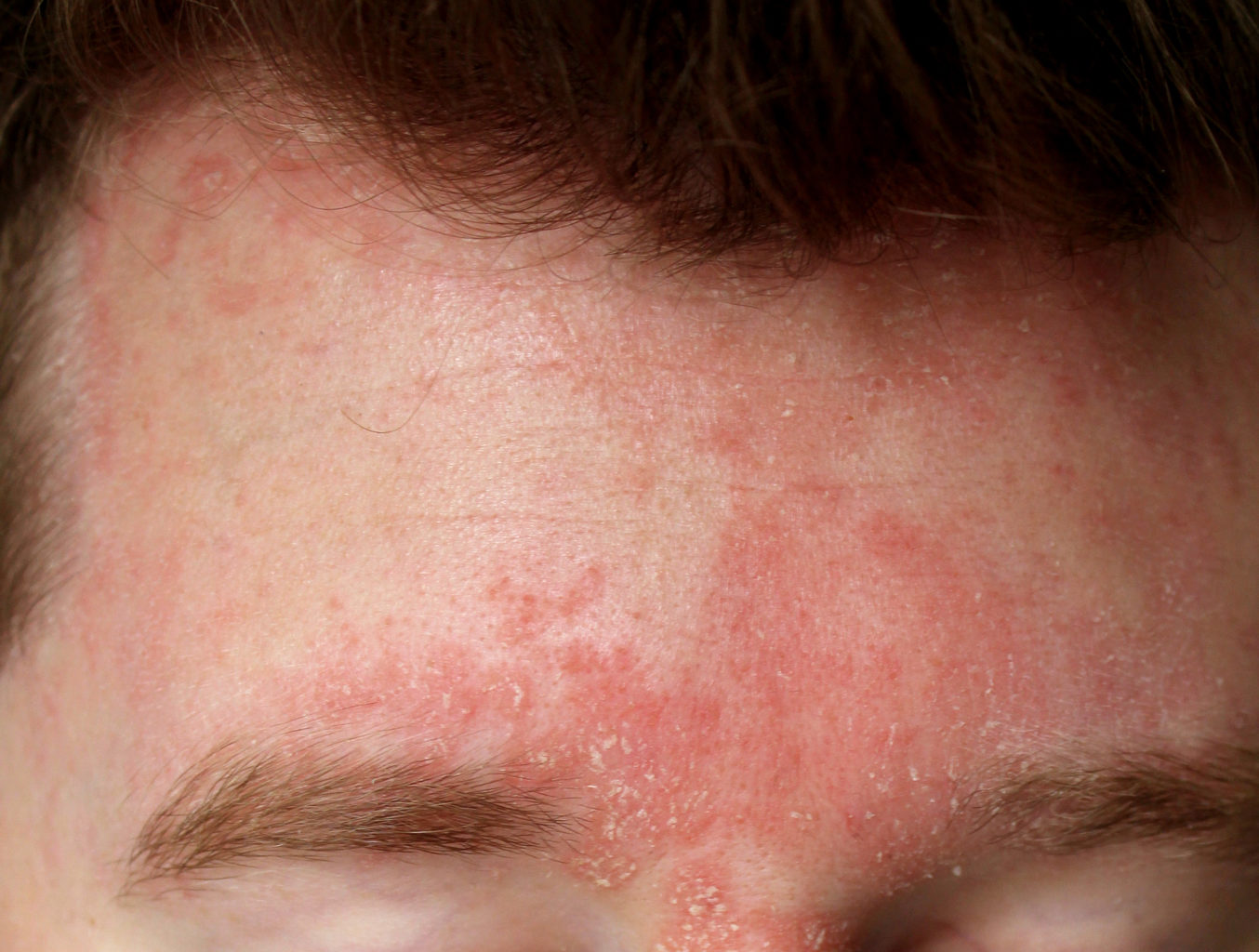
• Poorly defined greasy, scaly erythema, affecting the nasolabial folds and central
forehead.
• Fine scaling in the eyebrows, behind the ears, and within the ears (otitis externa), and/or
blepharitis.
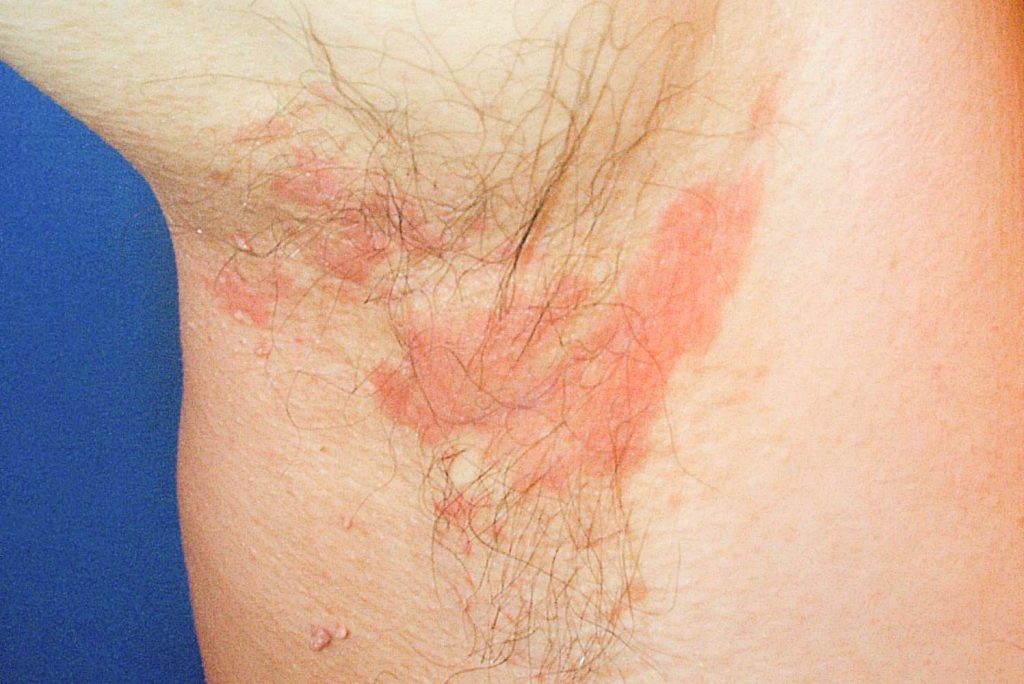
• Orangey, ill-defined erythema with fine scale in flexures (axillae, groin, umbilicus).
May resemble flexural psoriasis.
• Greasy, scaly, erythematous papules in the central chest and central back. May have an
annular configuration.
• Follicular papules or pustules over the back and sometimes the chest (pityrosporum
folliculitis).
• Normal nails—pitting suggests psoriasis.
• Erythroderma in severe disease.
What should I do?
It may be difficult to differentiate seborrhoeic dermatitis from flexural psoriasis
(sebopsoriasis), but the approach to management is similar. Consider HIV/AIDS in
patients with severe disease unresponsive to treatment. Treatment should tackle
inflammation, scaling, and over- growth of yeasts. treatment options include:
• Greasy emollient to use as a soap substitute and skin moisturizer.
• Hydrocortisone 1% ointment, combined with an imidazole, applied x1/day to the face
and flexures—combinations of a corticosteroid with an antifungal are more effective than
a corticosteroid alone.
• A moderately potent topical corticosteroid may be needed for a short time in the
flexures, e.g. trimovate® cream.
• Topical 0.1% tacrolimus ointment x1/day is an alternative to a mild corticosteroid for
facial or flexural seborrhoeic dermatitis.
• Ketoconazole shampoo for the scalp and as a body wash (useful in pityrosporum
folliculitis)—perhaps x2–3/week. Shampoo is drying and can irritate the skin—suggest
the use of a moisturizer.
• Alternative shampoos include preparations with tar or salicylic acid, e.g. Capasal®,
Polytar®, t-Gel®.
• A potent steroid lotion applied overnight may control scalp disease, e.g. Betnovate®
lotion or Dermovate® scalp application.