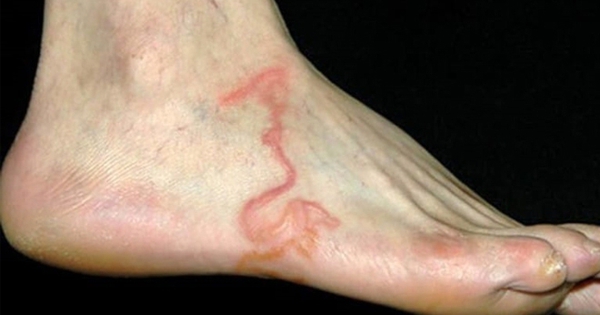
Synonym: creeping eruption
This parasitic skin disease is caused by hookworm larvae that usually infect domestic
animals. In their animal hosts, the larvae penetrate the skin to reach the blood and
lymphatic systems. They mature in the intestine. Eggs are excreted in faeces and take
about 7 days to hatch. The larvae are found on beaches and moist soils that have been
contaminated with animal faeces.
Cutaneous larva migrans presents in individuals whose skin has come into direct
contact with the larvae, e.g. walking barefoot or lying on sandy beaches. The larvae
tunnel through the stratum corneum into the epidermis but are unable to reach the
dermis in humans, because they can- not penetrate the basement membrane. The
disease is self-limiting, as humans are a ‘dead-end’ host.
Cutaneous larva migrans is usually acquired in tropical and subtropi- cal regions,
including the USa (south-eastern atlantic and Gulf coastal regions), the Caribbean,
South america, South East asia, and East and West africa.
What should I look for?
• The larvae migrate through the superficial epidermis, producing itchy, erythematous
linear or serpiginous tracks (creeping eruption).
• Tracks are often found on the feet but may be found on any skin surface that has
been in direct contact with larvae.
• The track elongates 1–2cm per day.
• Sometimes blisters develop around or within the tracks.
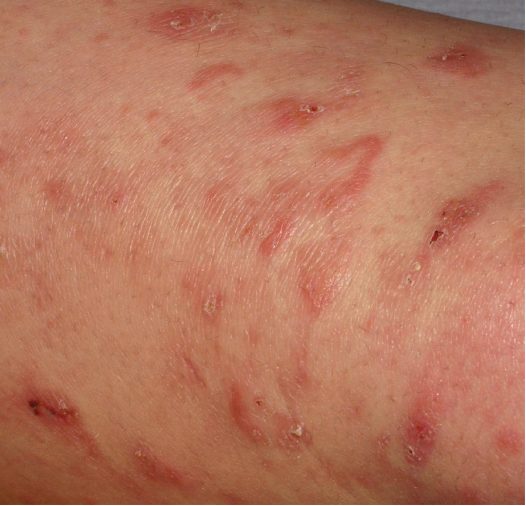
• Most patients have one or two tracks, but heavy infestations, e.g. in HIV/AIDS, are
associated with numerous itchy erythematous tracks, crusting, and 2° bacterial
infection.
What should I do?
• The diagnosis is based on the history and clinical findings.
• A skin biopsy is not helpful, as it is difficult to predict exactly where to
find the larva, which is somewhere just ahead of the leading edge of
the track.
• Antihelminth treatment options include:
Ivermectin: a single dose of 12mg or 200 micrograms/kg (available on a
named patient basis).
Albendazole: a single dose of 400mg or 400mg/day for 3–5 days for
widespread infection (available on a named patient basis).
Topical 10–15% tiabendazole solution: applied qds for 1 week under an
occlusive dressing (no commercial preparation available in the UK).
• Treat 2° bacterial infection.
• Prescribe a potent topical corticosteroid (apply bd) to reduce inflammation and
relieve itching.