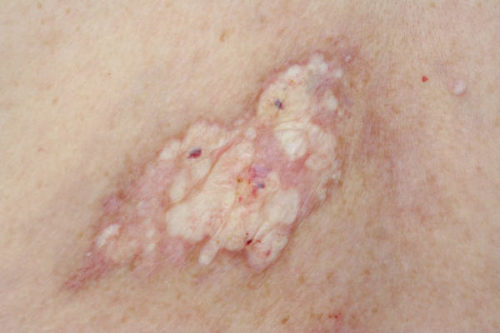
This chronic inflammatory disease with a predilection for genital skin has two peaks of
onset—childhood and post-menopausal. The cause is uncertain, but a lymphocyte-
mediated autoimmune pathogenesis is suspected. Lichen sclerosus may occur in
association with morphoea (with which extragenital lichen sclerosus shows considerable
clinical and histological overlap), LP, and vitiligo.
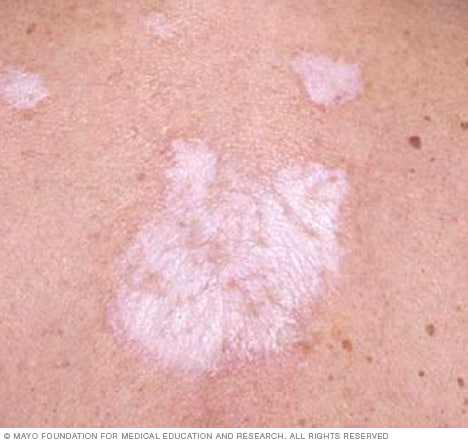
Lichen sclerosus is commonest in female adult. It may be asymptomatic but usually
presents with itch, pain, and/or dyspareunia. Perianal involvement with painful anal
fissures may lead to constipation in young girls. Uncircumcised male are affected. Lichen
sclerosus of the foreskin (balanitis zerotica obliterans) is a major indication for
circumcision. Lichen sclerosus may also develop around stomas, most often urostomies.
What should I look for?
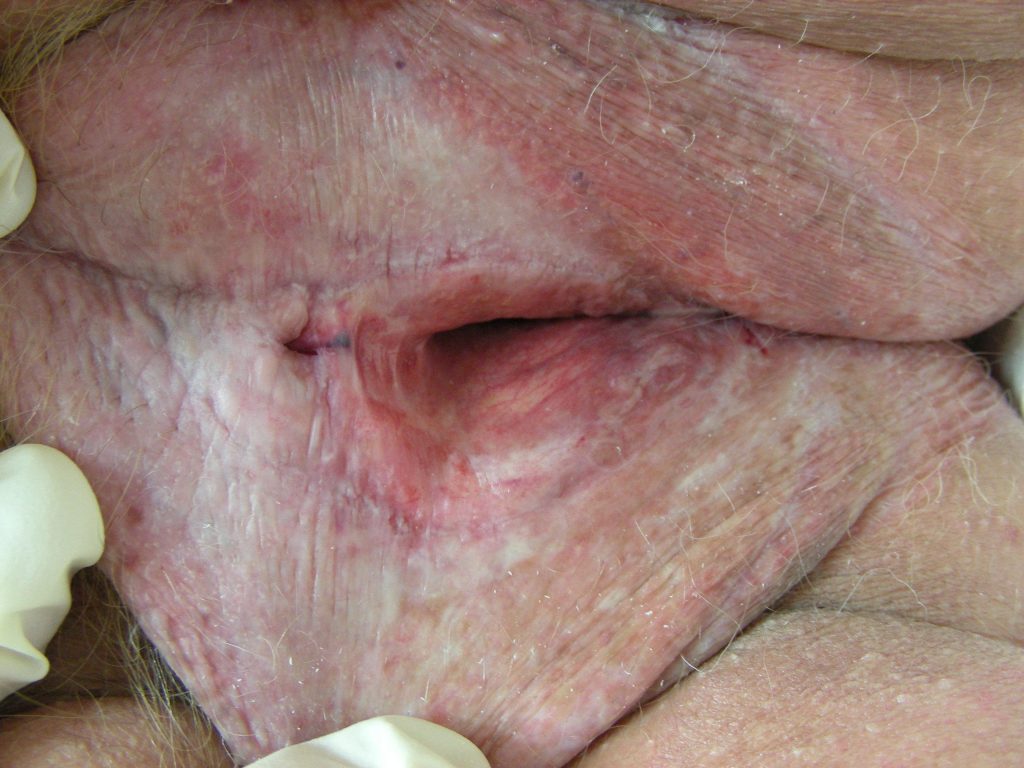
• Pearly white papules and plaques on labia minora, clitoris, and interlabial sulci.
• Sparing of the vulvar vestibule (unlike LP).
• Signs may extend in a figure-of-eight configuration to perianal skin in female (perianal
skin is not affected in male).
• Atrophy gives the skin a shiny crinkled appearance.
• Discrete areas of haemorrhage (ecchymoses) within the white plaques (may be
misdiagnosed as sexual abuse in young girls).
• Loss of normal anatomy in chronic disease—resorption of the labia minora, fusion of
the labia, and burying of the clitoris.
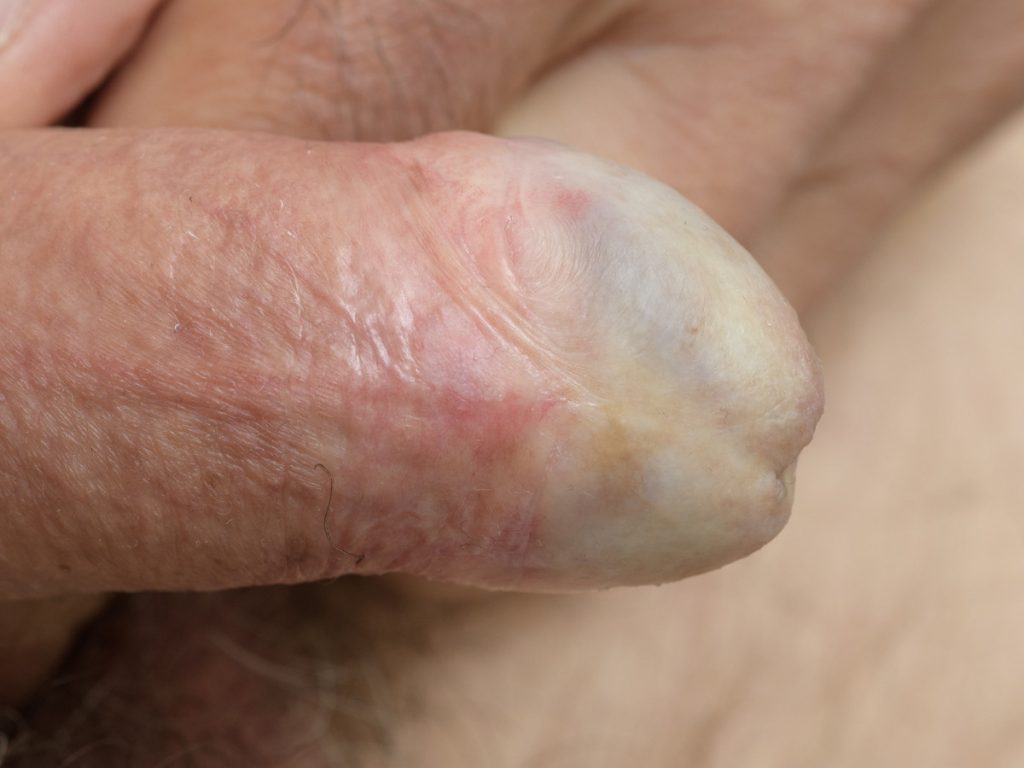
• Uncircumcised male—thickening and tightening of the foreskin, causing phimosis.
White plaques on the glans penis, sometimes with scarring. Sometimes pearly white
papules on the shaft of the penis.
• Extragenital lichen sclerosus is uncommon—the hypopigmented crinkled plaques
contain follicular plugs (unlike morphoea), ecchymoses, and rarely haemorrhagic blisters.
Hypopigmented papules are sometimes seen in children.
• SCC is a rare complication in chronic genital disease in adults (around 5% of patients).
Often presents with pain. Check for mucosal thickening, a nodule, or a persistent ulcer.
What should I do?
• Take a biopsy to confirm the diagnosis.
• Recommend a soap substitute for genital use, e.g. Cetraben® cream.
• A very potent topical corticosteroid (0.05% clobetasol propionate ointment), applied
x1/day for 4 weeks and then with gradually decreasing frequency for a further 8 weeks,
usually controls disease and may even reverse the early changes (may also be effective in
children).
• Counsel about the small risk of SCC; teach self-examination, and recommend annual
reviews.