Causes, incidence, and risk factors
Contact dermatitis is an inflammation of the skin caused by direct contact with an irritating or allergy-causing substance (irritant or allergen). Reactions may vary in the same person over time. A history of any type of allergies increases the risk for this condition.
Irritant dermatitis, the most common type of contact dermatitis, involves inflammation resulting from contact with acids, alkaline materials such as soaps and detergents, solvents, or other chemicals. The reaction usually resembles a burn.
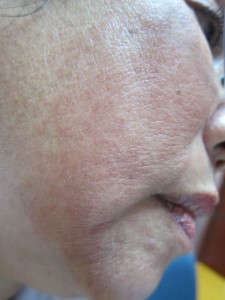
Allergic contact dermatitis, the second most common type of contact dermatitis, is caused by exposure to a substance or material to which you have become extra sensitive or allergic. The allergic reaction is often delayed, with the rash appearing 24 – 48 hours after exposure. The skin inflammation varies from mild irritation and redness to open sores, depending on the type of irritant, the body part affected, and your sensitivity.
Overtreatment dermatitis is a form of contact dermatitis that occurs when treatment for another skin disorder causes irritation.
Common allergens associated with contact dermatitis include:
– Poison ivy, poison oak, poison sumac
– Other plants
– Nickel or other metals
– Medication
+ Antibiotics, especially those applied to the surface of the skin (topical)
+ Topical anesthetics
+ Other medications
– Rubber or latex
– Cosmetics
– Fabrics and clothing
– Detergents
– Solvents
– Adhesives
– Fragrances, perfumes
– Other chemicals and substances
Contact dermatitis may involve a reaction to a substance that you are exposed to, or use repeatedly. Although there may be no initial reaction, regular use (for example, nail polish remover, preservatives in contact lens solutions, or repeated contact with metals in earring posts and the metal backs of watches) can eventually cause sensitivity and reaction to the product.
Some products cause a reaction only when they contact the skin and are exposed to sunlight (photosensitivity). These include shaving lotions, sunscreens, sulfa ointments, some perfumes, coal tar products, and oil from the skin of a lime. A few airborne allergens, such as ragweed or insecticide spray, can cause contact dermatitis.
Symptoms
– Itching (pruritus) of the skin in exposed areas
– Skin redness or inflammation in the exposed area
– Tenderness of the skin in the exposed area
– Localized swelling of the skin
– Warmth of the exposed area (may occur)
– Skin lesion or rash at the site of exposure
+ Lesions of any type: redness, rash, papules (pimple-like), vesicles, and bullae (blisters
+ May involve oozing, draining, or crusting
+ May become scaly, raw, or thickened
Signs and tests
The diagnosis is primarily based on the skin appearance and a history of exposure to an irritant or an allergen.
According to the American Academy of Allergy, Asthma, and Immunology, “patch testing is the gold standard for contact allergen identification.” Allergy testing with skin patches may isolate the suspected allergen that is causing the reaction.
Patch testing is used for patients who have chronic, recurring contact dermatitis. It requires three office visits and must be done by a clinician with detailed experience in the procedures and interpretation of results. On the first visit, small patches of potential allergens are applied to the skin. These patches are removed 48 hours later to see if a reaction has occurred. A third visit approximately 2 days later is to evaluate for any delayed reaction. You should bring suspected materials with you, especially if you have already tested those materials on a small area of your skin and noticed a reaction.
Other tests may be used to rule out other possible causes, including skin lesion biopsy or culture of the skin lesion (see skin culture or mucosal biopsy culture).
Treatment
Initial treatment includes thorough washing with lots of water to remove any trace of the irritant that may remain on the skin. You should avoid further exposure to known irritants or allergens.
In some cases, the best treatment is to do nothing to the area.
Corticosteroid skin creams or ointments may reduce inflammation. Carefully follow the instructions when using these creams, because overuse, even of low-strength over-the-counter products, may cause a troublesome skin condition. In severe cases, systemic corticosteroids may be needed to reduce inflammation. These are usually tapered gradually over about 12 days to prevent recurrence of the rash. In addition to or instead of corticosteroid skin treatment, your doctor may prescribe tacrolimus ointment or pimecrolimus cream.
Wet dressings and soothing anti-itch (antipruritic) or drying lotions may be recommended to reduce other symptoms.
Expectations (prognosis)
Contact dermatitis usually clears up without complications within 2 or 3 weeks, but may return if the substance or material that caused it cannot be identified or avoided. A change of occupation or occupational habits may be necessary if the disorder is caused by occupational exposure.
Complications
Secondary bacterial skin infections may occur.
Calling your health care provider
Call your health care provider if symptoms indicate contact dermatitis and it is severe or there is no improvement after treatment.
Prevention
Avoid contact with known allergens. Use protective gloves or other barriers if contact with substances is likely or unavoidable. Wash skin surfaces thoroughly after contact with substances. Avoid overtreating skin disorders.
References
- Gober MD, DeCapite TJ, Gaspari AA. Contact dermatitis. In: Adkinson NF Jr, ed. Middleton’s Allergy: Principles and Practice. 7th ed. Philadelphia, Pa: Mosby Elsevier; 2008:chap 63.
- Habif TP. Contact dermatitis and patch testing. In: Habif TP, ed. Clinical Dermatology. 5th ed. Philadelphia, Pa: Mosby Elsevier; 2009:chap 4.